Our Mission
Our Services
Compassionate Care Meets Advanced Sleep Testing in Ormeau
At NHHPCO, we are committed to enhancing the quality of life for individuals and families by providing compassionate care and essential health support. From palliative services to holistic wellness solutions, our mission is to guide patients through every stage of their healthcare journey with dignity and understanding. We work closely with local professionals to address not only physical needs but also emotional and lifestyle factors that influence overall well-being.
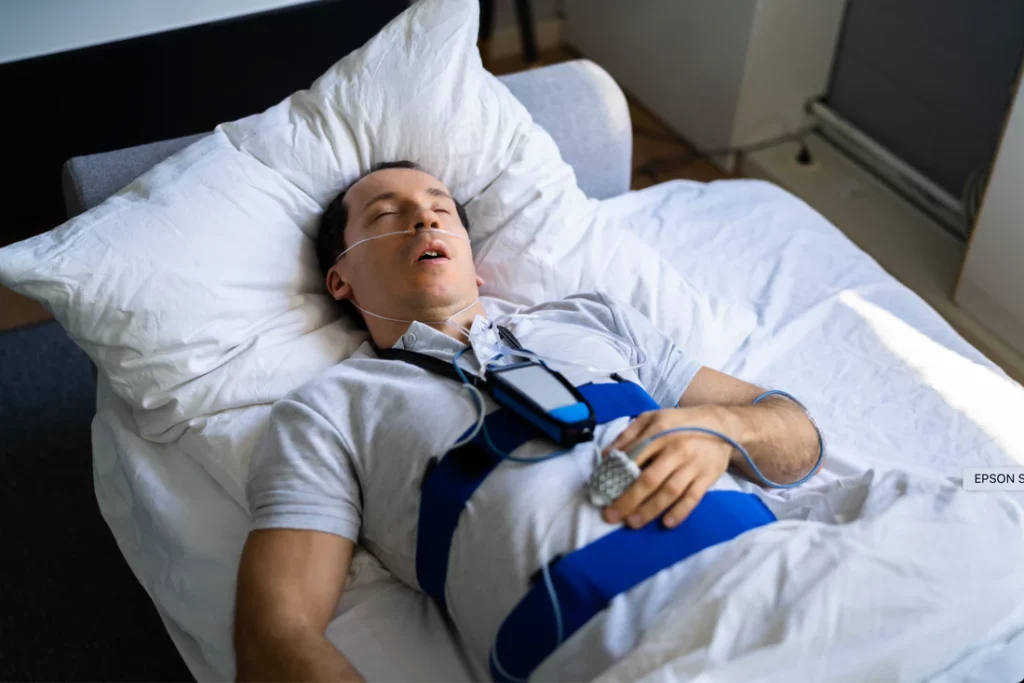
As part of our broader care approach, we proudly connect visitors with specialized services such as sleep testing Ormeau—a crucial step for individuals experiencing disrupted sleep patterns, fatigue, or possible sleep disorders. Early diagnosis through sleep testing can greatly improve treatment outcomes and long-term health. Whether you’re a caregiver or patient, knowing where to turn for expert sleep assessment is just one way we help families access the support they need.

Why Choose NHHPCO
01
Expert Support
Access a network of skilled hospice and palliative care professionals dedicated to providing compassionate and personalized end-of-life support.
02
Educational Resources
Discover valuable guides and information designed to empower families and caregivers during difficult times in their caregiving journey.
03
Community Advocacy
Engage in initiatives aimed at enhancing end-of-life care standards and increasing awareness for compassionate support across Australia.
What People Say About Us
Recent Posts
How a Sleep Study Machine Tracks Your Breathing Overnight
Most people picture one device doing everything, but “sleep study machine” usually means a set…
Private Sleep Study Cost vs Public Options: Which Is Better?
Private options can be faster and more flexible, while public pathways can be far cheaper….
Natural Remedies for Sleep Apnea: Do They Really Work?
Sleep apnea is a serious sleep disorder that can leave you tired after sleeping, even…
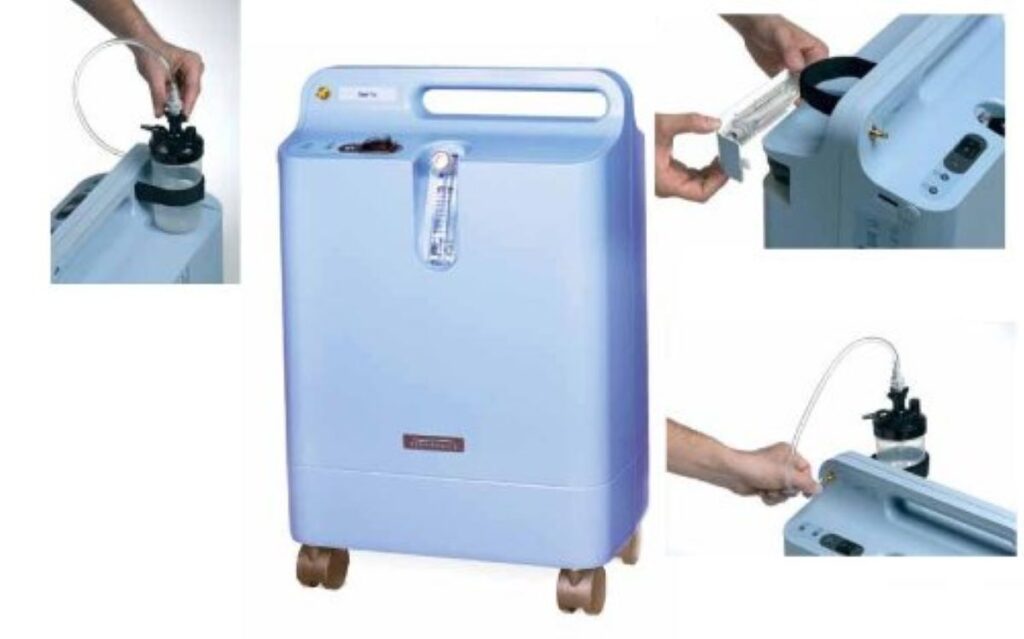
Top 5 Reasons the EverFlo Oxygen Concentrator Is Popular in Australia
What Makes the EverFlo Oxygen Concentrator a Trusted and Low-Maintenance Solution? The EverFlo Oxygen Concentrator…
Philips EverFlo Oxygen Concentrator Australia: Where to Buy and Warranty Info
Where Can Australians Buy the Philips EverFlo Oxygen Concentrator? Australians can purchase the Philips EverFlo…
Understanding Pilates Care
What Is Palliative Care? (from the Center to Advance Palliative Care) Palliative care is specialized medical…